HSV2 genital herpes infections tend to be more severe than HSV-1 infections and are more likely to occur during recurrent or subclinical viral shedding. Infections with HSV-2 usually occur during intercourse and are most common among sexually active adults and teenagers. This infection is spread most commonly through intercourse with multiple partners and is rarely found in children. People at risk for HSV-2 infection include women of the Hispanic or black race, high-risk sexual intercourse, and co-infection with another STD. Infection is also more likely to occur in patients between 15 and 30 years of age.
Treatment is dependent on the individual’s level of infection. Some people experience only a single outbreak in their lifetime, while others have recurrent outbreaks several times a year. While there is no vaccine or treatment for HSV-2, prevention is key. Patients should practice good hygiene and limit contact with sexual partners with lesions. They should avoid sharing grooming utensils or kissing. They should also refrain from sexual activity for a while to minimize the spread of the virus. Get in touch with Herpecillin for a Genital Herpes cure.
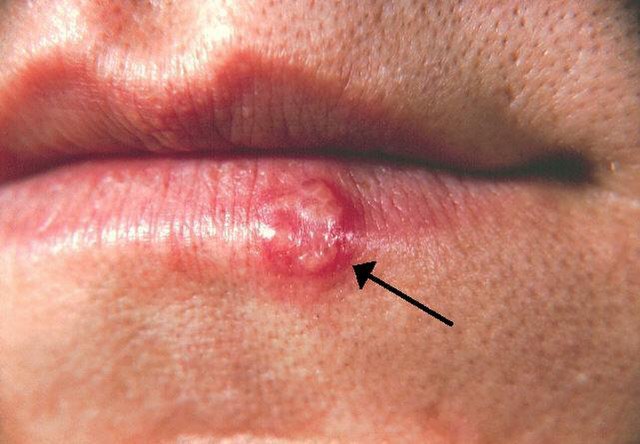
In some cases, the virus is not infectious and causes no symptoms. However, in others, it may cause painful ulcers in the genitals or rectum. Those who suffer from herpes should be aware that first outbreaks are usually worse than subsequent ones. A physical exam, blood tests, and a herpes lesion swab can help determine whether an individual has genital HSV-2. Antiviral medication may be recommended to reduce the frequency of outbreaks. Support groups are also available to educate individuals about the disease and offer treatment options.
Research is revealing more information about HSV-1 and HSV-2. The latest advances in medicine may lead to a vaccine for HSV2 genital herpes and cold sores. Staying abreast of research on HSVs is essential for those who have the disease. It will allow researchers to find a treatment that will stop recurrences and prevent cold sores.
PCR is used to diagnose HSV infection in patients with fresh lesions. The direct immunofluorescence assay is fast and accurate, but it has less sensitivity than the PCR and can only identify the presence of HSV type 2 in fresh lesions. Viral culture has been the gold standard of HSV2 genital herpes diagnosis until recently. Viral culture is a highly specific test for HSV but is limited by inappropriate sample handling.
HSV infection can be lifelong, with the virus remaining in nerve cells, so make sure to go for a herpes cure. In addition to the outbreaks, HSV-related symptoms include tingling and itching, sores around the mouth, and swollen lymph nodes. Some people experience periodic outbreaks, while others may not exhibit any symptoms at all. It is important to see a doctor as soon as you suspect herpes.
When pregnant, women with HSV2 genital herpes should inform their physician. Taking antiviral medication during pregnancy may reduce the risk of transmitting the virus to the unborn baby. During delivery, doctors may also opt to deliver the baby by cesarean section. Nevertheless, prevention is still the best option. Using condoms and barrier methods will help to minimize the risk of infection and its symptoms.
When it comes to herpes, there are two kinds. Type 1 can be transmitted by oral secretions, whereas HSV-2 can only be transmitted through sexual contact with a person with genital HSV-2. Although HSV-1 can be spread through oral-to-oral contact, herpes from a mother’s genital HSV-2 infection can be passed on to the unborn child during childbirth.
Although HSV2 genital herpes is often transmitted to children, it can be passed to adults in the same household. In the U.S., 16.2 percent of people between the ages of fifteen and forty-nine are infected with HSV-2. And the number of people with the infection has remained relatively stable over the past decade. However, some people don’t notice any symptoms.